When you have type 1 diabetes you know that the problem is not just high glucose.The true origin is in the immune system, which for some reason decides to attack the beta cells of the pancreas, those responsible for producing insulin.This progressive destruction is what forces us, from the very beginning, to live dependent on a hormone that our own body can no longer manufacture.
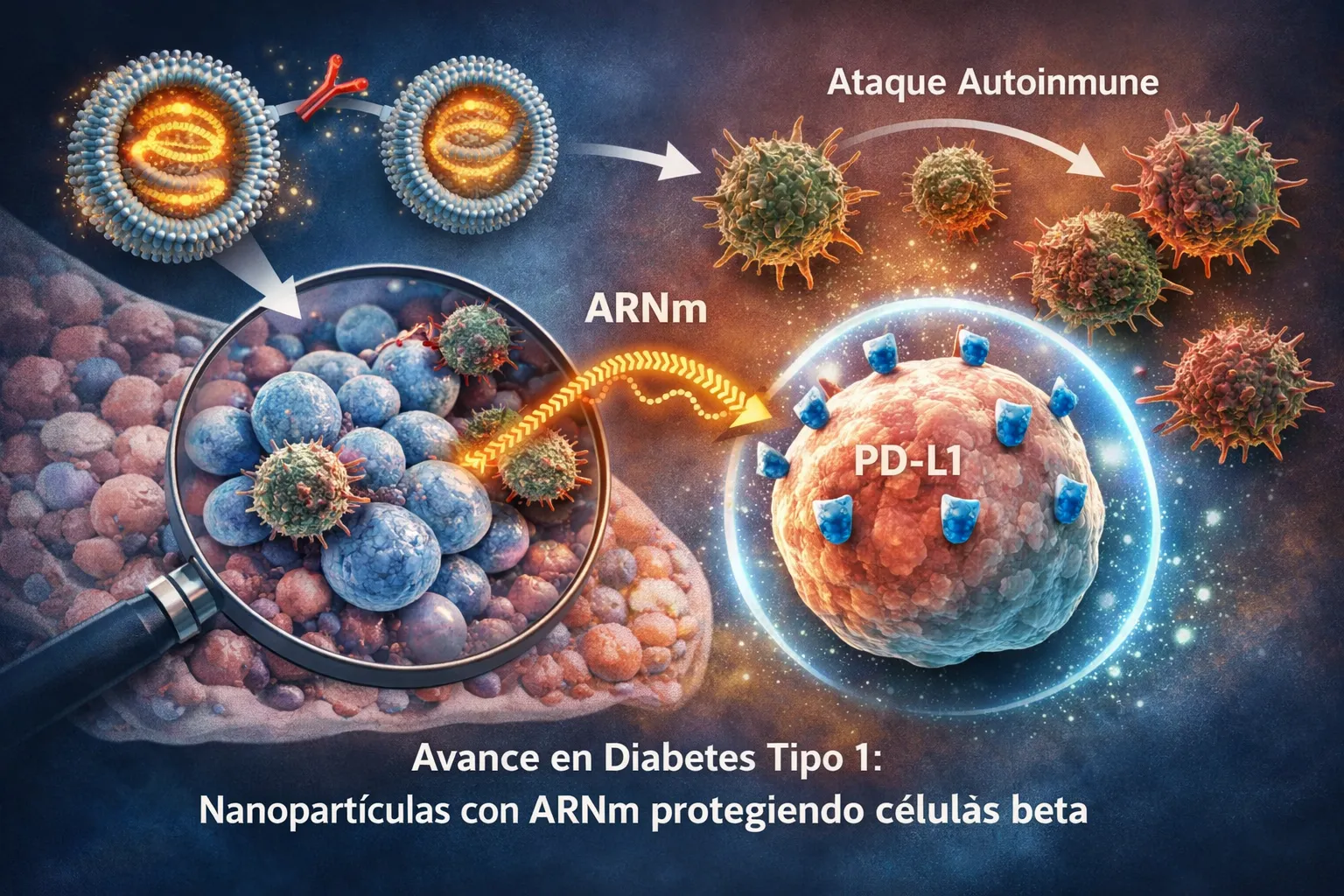
That is why it is so encouraging to read research that does not focus solely on replacing insulin, but on protecting the beta cells that still exist or preserving those that can be transplanted in the future.A team from the University of Chicago has published a study in Cell Reports Medicine in which they use lipid nanoparticles to transport mRNA to beta cells and get them to express a protein called PD-L1.This protein acts as a brake on the immune system, limiting the activity of T lymphocytes and reducing tissue damage.
The technology used is similar to that used in some vaccines against COVID-19, but here the objective is not to activate defenses, but quite the opposite: to help insulin-producing cells to partially “hide” from the autoimmune attack.In experimental models with mice and also in human cells, the nanoparticles were able to specifically reach beta cells and induce the expression of PD-L1.A delay in the progression of type 1 diabetes was observed in animals, which opens the door to new therapeutic strategies.
The interesting thing is that the researchers designed versions specifically targeting receptors present on beta cells, such as the GLP-1 receptor, increasing the precision of the treatment and minimizing effects on other tissues.This ability to act selectively is key to avoiding unwanted consequences in the rest of the body.
Does this mean that we are facing a cure?No.
It is important to remain cautious.This is a proof of concept in experimental models and there is still a long way to go before something like this can be widely applied to people.But change the focus.Instead of simply compensating for the lack of insulin, we try to intervene in the autoimmune process that destroys beta cells.
For those of us who live with type 1 diabetes, reading about these types of advances has an emotional impact.We have all thought at some point what our lives would have been like if autoimmune destruction could have been stopped in the early stages.Imagining treatments that delay or stop this process is not a fantasy, it is a real line of research that is evolving.
Meanwhile, our reality continues to be that of counting carbohydrates, adjusting doses, managing hypoglycemia and monitoring arrows on the sensor.But knowing that science is exploring ways to protect our own insulin-producing cells reminds us that the story of type 1 diabetes is not closed.Research advances, and every small step towards preserving beta cells is a step towards a future with less daily burden and more freedom.